In most cases, patients with a herniated lumbar disc improve with conservative treatments, including anti-inflammatory medications, painkillers and physical therapy. But when conservative treatment methods are not enough, lumbar spine surgery can help patients with low-back pain find relief and get back to living a normal life.
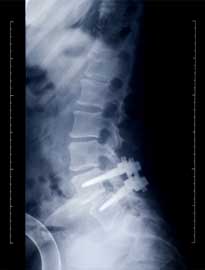
Dr. Foroohar performs several lumbar spine surgery procedures to treat herniated discs, as well as spinal stenosis and back injuries.
Why choose a neurosurgeon for back surgery?
Microdiscectomy—A minimally invasive surgery that involves removing a lumbar herniated disc through a tiny incision using a microscope. The surgery is usually done on an outpatient basis, and patients can go home the same day.
Lumbar laminectomy—A surgical procedure to remove part of the spine known as the lamina in the lower back. Dr. Foroohar performs this surgery, with or without lumbar fusion, to relieve spinal stenosis.
Lumbar fusion—A surgical procedure to join or fuse two or more vertebrae with bone graft, synthetic bone graft substitutes, and bone growth factors and hardware including pedicle screws, rods and cages. There are many different ways to do a lumbar fusion.
Lumbar fusion is done when there is spinal mechanical instability in the lower back, such as spondylolisthesis. Dr. Foroohar performs lumbar fusion surgery in partnership with an orthopedic surgeon for complicated cases.
Anterior and posterior lumbar interbody fusion—This surgical procedure removes the disc entirely and replaces it with an implant such as a bone graft or a cage packed with bone graft. This implant is placed in the inner space of the disc; then the bone graft or cage will fuse with the vertebral body.
What is involved in a microdiscectomy?
We go in posteriorly—from the back—and usually take down the muscle on one side and do a hemilaminotomy, which is removing a small portion of the bone. Then we do the microdiscectomy to remove the disc and relieve the lumbar nerve root being pinched by the herniated disc.
How soon can patients go home after a microdiscectomy?
A microdiscectomy is a minimally invasive procedure with a very small incision. Most patients can go home the same day.
How does lumbar fusion surgery differ from doing a neck or upper-back fusion?
Doing a lumbar fusion is very different from doing a cervical fusion in terms of the skill set and the hardware involved. When we fuse the lumbar spine, we have to put in screws through the pedicle, which is the small bone that connects the bones in the back of the spine to the vertebral body.
Putting in the screws is an intricate process because you can see only the surface where the screw is entering, but you're putting in a three-dimensional device. So the trajectory or path of how you put this in requires very specialized skill.
With cervical fusion, we're not putting screws in a pedicle; we're putting a screw in the vertebral body or facets.
Is lumbar fusion used to treat a fracture in the lower back?
Yes. In some cases, we need to do a lumbar fusion to treat a fracture in the low back.
What does lumbar fusion typically treat?
We tend to do lumbar fusion in patients who have mechanical instability—whether due to lumbar spondylolisthesis, prior surgery such as laminectomy or discectomy, or scoliosis.
In patients who have had a laminectomy and have scoliosis, lumbar fusion can help prevent further instability by keeping the spinal curvature from getting worse.
A patient could have a slippage in the spine—known as spondylolisthesis. In these patients, we would definitely do a fusion because if we remove the bone, the spine is just going to slip more and worsen the instability.
How do you avoid damaging delicate nerves during spinal surgery?
For all spinal surgery, we do intraoperative nerve monitoring. We have a neurophysiologist who monitors the nerves live during surgery. That information is sent to a neurologist who is live and following the procedure.
If something happens during surgery, the intraoperative nerve monitoring would tell us if the nerve is not functioning right. The monitoring is somatosensory evoked-potential, or SSEP, which assesses the function of the patient's spinal cord and nerves by stimulating peripheral nerves and recording the response from the patient's scalp.
And when we put in the screws during a lumbar fusion, we do an EMG to make sure we're not hitting a nerve.
Is there a general term for degenerative spinal conditions?
Yes. Spondylosis is a blanket term for arthritis and degenerative disease of the spine, whether the specific diagnosis is a herniated disc, stenosis, spondylolisthesis, scoliosis or another condition.
What effect can trauma have on these spinal conditions?
A traumatic injury can aggravate any pre-existing lower-back condition. For example, if you have a herniated disc or spinal stenosis and then are involved in a motor vehicle accident, the trauma of the accident will just make your underlying problem worse.
In cases like that, the trauma is obviously not what caused the lower-back condition—it just exacerbated the original condition.